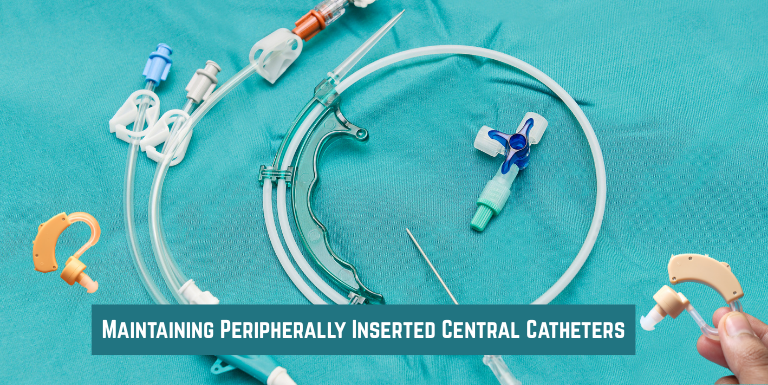
A Peripherally Inserted Central Catheter (PICC) is a critical medical device used for intravenous access in patients who require prolonged treatment, such as chemotherapy, antibiotics or parenteral nutrition. PICC lines are typically inserted into a peripheral vein and advanced toward the central venous system, offering a more comfortable and less invasive option compared to traditional central venous catheters. The PICC kit – comprising all the necessary components for insertion – ensures proper placement and secure connection for safe and effective treatment.
However, the longevity and efficiency of these catheters rely heavily on proper maintenance. Without regular care, complications such as infections, occlusions and catheter malposition can occur, compromising patient safety. This article outlines best practices for maintaining PICC lines, emphasizing essential techniques that help healthcare providers ensure these devices function optimally over time, reducing risks and improving patient outcomes.
Routine Inspection of the Catheter and Insertion Site
Regular inspection is fundamental to maintaining the function and safety of a PICC line. Healthcare providers should visually inspect both the catheter and the insertion site for signs of infection, such as swelling, redness or drainage. The catheter should also be checked for any visible damage, such as cracks or kinks, that could compromise its function.
Additionally, signs of displacement or misplacement must be promptly addressed. A central venous catheter kit often includes a securement device that helps keep the catheter in place, but frequent checks are still necessary to ensure it remains positioned correctly. If the catheter appears to have shifted, medical staff may need to reposition it or replace the PICC line to avoid further complications.
Maintaining Aseptic Technique During Care
Aseptic technique is one of the most important aspects of PICC line maintenance to prevent infection, especially catheter-related bloodstream infections (CRBSIs). Every time the catheter is accessed for blood draws, medication infusion or dressing changes, healthcare workers must strictly adhere to sterile procedures. This includes washing hands thoroughly, wearing sterile gloves and ensuring that all components – such as syringes, flush solutions and dressings – are sterile.
PICC kit components should be used as instructed, with particular attention to the sterilization of the insertion site and dressing. Regular dressing changes, typically every 7 days or sooner if soiled, reduce the risk of bacterial contamination at the insertion site. This process is critical for preventing infection and ensuring that the peripherally inserted central catheter functions effectively without introducing harmful pathogens.
Flushing Protocols to Maintain Patency
One of the most common issues with PICC lines is catheter occlusion, which can occur due to the formation of clots. Regular flushing is necessary to prevent these clots from forming and to maintain catheter patency. Flushing should be done with either saline or heparinized saline, depending on the patient’s condition and treatment plan.
The flush procedure typically follows the push-pause method, a technique that helps clear the catheter by creating pressure while allowing for intermittent pauses to prevent over-pressurization. PICC lines should be flushed after each use – whether it’s for medication, a blood draw or at least once a day if the catheter is unused. Following a well-defined flushing protocol reduces the risk of occlusions and ensures that the catheter remains functional throughout its use.
Preventing Catheter Dislodgement
Dislodgement of the PICC line can result in complications such as misplacement, which can interfere with the catheter’s function and lead to treatment delays. To prevent dislodgement, it is essential to properly secure the catheter at the insertion site. Transparent dressings and securement devices should be used to prevent the catheter from moving or being inadvertently pulled during patient activity.
In addition to securement, patients must be educated on how to protect the catheter. Activities such as lifting heavy objects or participating in vigorous exercise can place unnecessary strain on the PICC line. Educating the patient about the importance of avoiding excessive tugging or pressure on the catheter is essential for maintaining its position and functionality.
Monitoring for Complications
Regular monitoring of the PICC line and insertion site is essential for detecting complications early. Healthcare providers should be vigilant for signs of infection, thrombosis or occlusion. If resistance is encountered while flushing or if there is an inability to obtain blood return, these may be signs of clotting or catheter malfunction.
The healthcare team should also be mindful of changes in the patient’s condition that could affect catheter function. For example, changes in the patient’s clinical status – such as fever, chills or swelling around the insertion site – may indicate a developing infection. Early identification of such issues can lead to prompt intervention, such as the administration of antibiotics or the decision to replace the central venous catheter kit if necessary.
Documenting and Reporting Maintenance Activities
Comprehensive documentation is an essential part of PICC line management. Healthcare providers should record all maintenance activities, including catheter checks, dressing changes, flushes and any incidents or complications. Proper documentation allows for continuity of care, especially when multiple providers are involved and helps ensure that no essential procedures are overlooked.
This record-keeping should also include any changes in the patient’s condition, the catheter’s status or interventions performed. It provides a detailed history of the peripherally inserted central catheter’s usage and helps identify any trends that might require adjustments in treatment.
Removal and Replacement Protocols
PICC lines are designed for long-term use, but they do have a limited lifespan. If complications arise or if the catheter becomes infected, blocked or damaged, it may need to be replaced or removed. PICC kit manufacturers provide guidelines on the appropriate duration of catheter use, but healthcare providers should assess the need for replacement on a case-by-case basis, depending on factors like patient condition and the presence of complications.
Catheters should also be removed when no longer needed for treatment. The removal process should be done following strict protocols to minimize the risk of complications, such as accidental dislodgement or infections. Proper care during the removal process ensures that the patient’s treatment continues without interruption and reduces the potential for complications.
Maintaining Peripherally Inserted Central Catheters (PICC) requires consistent, diligent care to ensure that these devices continue to function properly throughout their use. By adhering to best practices such as routine inspection, aseptic technique, regular flushing and continuous monitoring for complications, healthcare providers can greatly reduce the risk of infection, occlusion and dislodgement.
Proper maintenance of PICC lines is vital to ensuring that patients receive safe, effective treatment and that the catheters remain functional for extended periods. Utilizing the tools provided in the PICC kit, including securement devices, flush solutions and sterile dressings, can significantly contribute to the success of the catheter and prevent complications.
By following these best practices, healthcare providers can ensure the PICC line serves its intended purpose without complications, ultimately improving patient outcomes and contributing to the overall success of intravenous therapies.

We are recognized as one of the leading manufacturers, exporters, and suppliers of a diverse range of high-quality medical devices in India. Our products, including Interventional Cardiology, Nephrology, Anaesthesia, General Consumables, and Critical Care Accessories, are designed to meet the highest standards of excellence, ensuring reliable performance and patient care.
A – 8, Kuraopokpi industrial Estate,
Thoubal (kakching) Imphal,
Manipur – 795001, India.